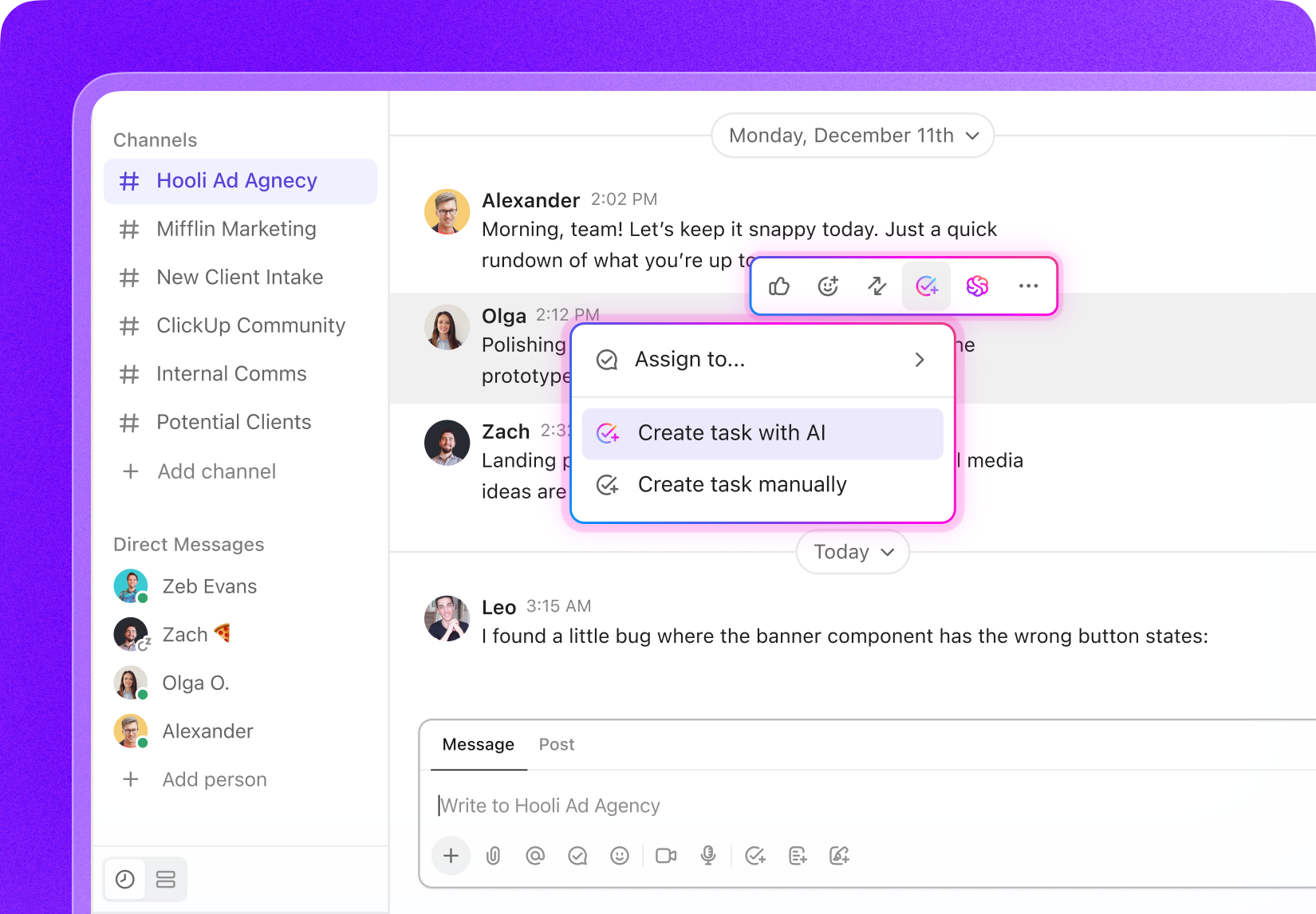
Task Software Tailored for Medical Claims Processing
Task Management Software Designed for Medical Claims Processors
Consolidate your claims workflows, monitor submission statuses, collaborate effortlessly with your team, and maintain full oversight of every claim stage.
Trusted by the best
The Challenge of Managing Claims
Why Medical Claims Processors Need Dedicated Task Management Software
Handling medical claims without a streamlined system results in lost details, fragmented data, and workflow bottlenecks — turning routine tasks into major hurdles.
- Complex claim timelines cause delays — it’s tough to track approvals, denials, and resubmissions effectively.
- Patient records scatter easily — critical information gets misplaced across various systems.
- Manual error risks increase — missing documentation or incorrect coding leads to costly rejections.
- Collaboration between departments stalls — unclear task ownership and communication gaps slow processing.
- Deadlines for claim submissions are missed — leading to lost reimbursements and compliance issues.
- Progress tracking feels opaque — it’s hard to get a real-time view of claim statuses.
- Communication breakdowns occur — reliance on emails and calls makes alignment difficult.
- Resource allocation conflicts arise — overlapping workloads and priorities disrupt efficiency.
Traditional Systems vs ClickUp
Why Conventional Claim Management Falls Short
Discover how ClickUp brings transparency and control that legacy tools lack.
Traditional Methods
- Tasks scattered across spreadsheets, emails, and paper files
- Claim details duplicated or lost amid systems
- Manual tracking with high potential for errors
- Poor coordination between billing, coding, and audit teams
- Submission deadlines often overlooked
- Patient and claim data spread across disconnected platforms
ClickUp Task Management
- Centralized claims with clear status indicators and priorities
- Organized patient records linked directly to tasks
- Automated workflows minimizing manual entry and errors
- Transparent task assignments and real-time team collaboration
- Reminder systems and calendar syncing for every deadline
- Searchable documentation and audit trails within each task
Use cases
Unlock How Task Management Software Empowers Medical Claims Processors
See how task organization cuts confusion and streamlines claim resolution.
#UseCase1
Consolidating Claim Data Across Departments and Systems
Patient info, billing codes, and insurance details stay centralized—ClickUp links all files and notes within the relevant claim tasks for easy access.
#UseCase2
Maintaining a Clear Audit Trail for Compliance and Reviews
Compliance is critical. ClickUp records every claim update, comment, and attachment, ensuring every action is documented and traceable.
#UseCase3
Managing Evolving Payer Feedback Without Losing Track
Insurance responses often change, but ClickUp captures feedback and status changes with comments and version history, keeping your team aligned.
#UseCase4
Preventing Processing Errors Through Standardized Workflows
Complex claim steps can cause errors, but ClickUp’s templates, checklists, and dependencies enforce consistency and accuracy every time.
#UseCase5
Tracking Submission Deadlines and Appeal Windows Reliably
Appeals and submissions have strict timelines—ClickUp’s reminders and custom fields ensure no deadline is missed.
#UseCase6
Coordinating Resource Allocation Across Claims and Teams
Claims often compete for limited staff and resources; ClickUp visualizes workloads and dependencies to optimize task distribution.
#UseCase7
Avoiding Duplicate Claims and Billing Errors
Duplicate submissions waste time and money—ClickUp tags and filters prevent repeats and track claim statuses clearly.
#UseCase8
Streamlining Communication Between Coding, Billing, and Auditing
ClickUp centralizes messages, tasks, and files so teams collaborate efficiently, reducing back-and-forth delays.
#UseCase9
Turning Team Meetings Into Clear, Actionable Plans
Meeting discussions become assigned tasks with deadlines and checklists, ensuring follow-through and accountability.
Key Beneficiaries
Who Gains the Most from ClickUp in Medical Claims Processing
For claims teams seeking a unified platform to manage complex workflows and improve accuracy.
If you’re a Claims Processor
ClickUp helps you streamline claim tracking, reduce errors, and meet strict submission deadlines without juggling multiple tools.
If you’re a Billing Specialist
ClickUp standardizes billing workflows, maintains accurate coding documentation, and facilitates smooth communication with payers.
If you’re an Audit Coordinator
ClickUp provides a clear audit trail, tracks compliance tasks, and organizes documentation for regulatory reviews.
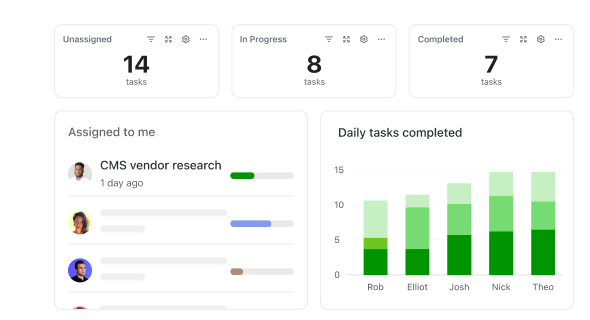
How ClickUp Supports Medical Claims Processing
Step-by-Step: Simplify Each Claim Stage
Manage patient data, billing codes, and approvals without switching platforms.
Centralize Patient and Claim Information
Keep all medical records, insurance details, and billing codes in one accessible workspace—no more lost paperwork.
Plan Claims Through Defined Stages
Segment workflows into submission, review, appeal, and payment phases using task lists and timelines.
Standardize Claim Review and Submission
Use templates and checklists to ensure all documentation and coding is accurate and compliant.
Collaborate Seamlessly Across Teams
Assign tasks to coders, billers, and auditors with shared dashboards to keep everyone aligned.
Convert Meetings Into Actionable Tasks
Turn strategy discussions into tasks with owners, deadlines, and progress tracking.
Stay Ahead of Deadlines and Compliance
Automate reminders for claim submissions, appeals, and audits with calendar integrations.