Elevate Medical Claims Management with the Leading CRM Software
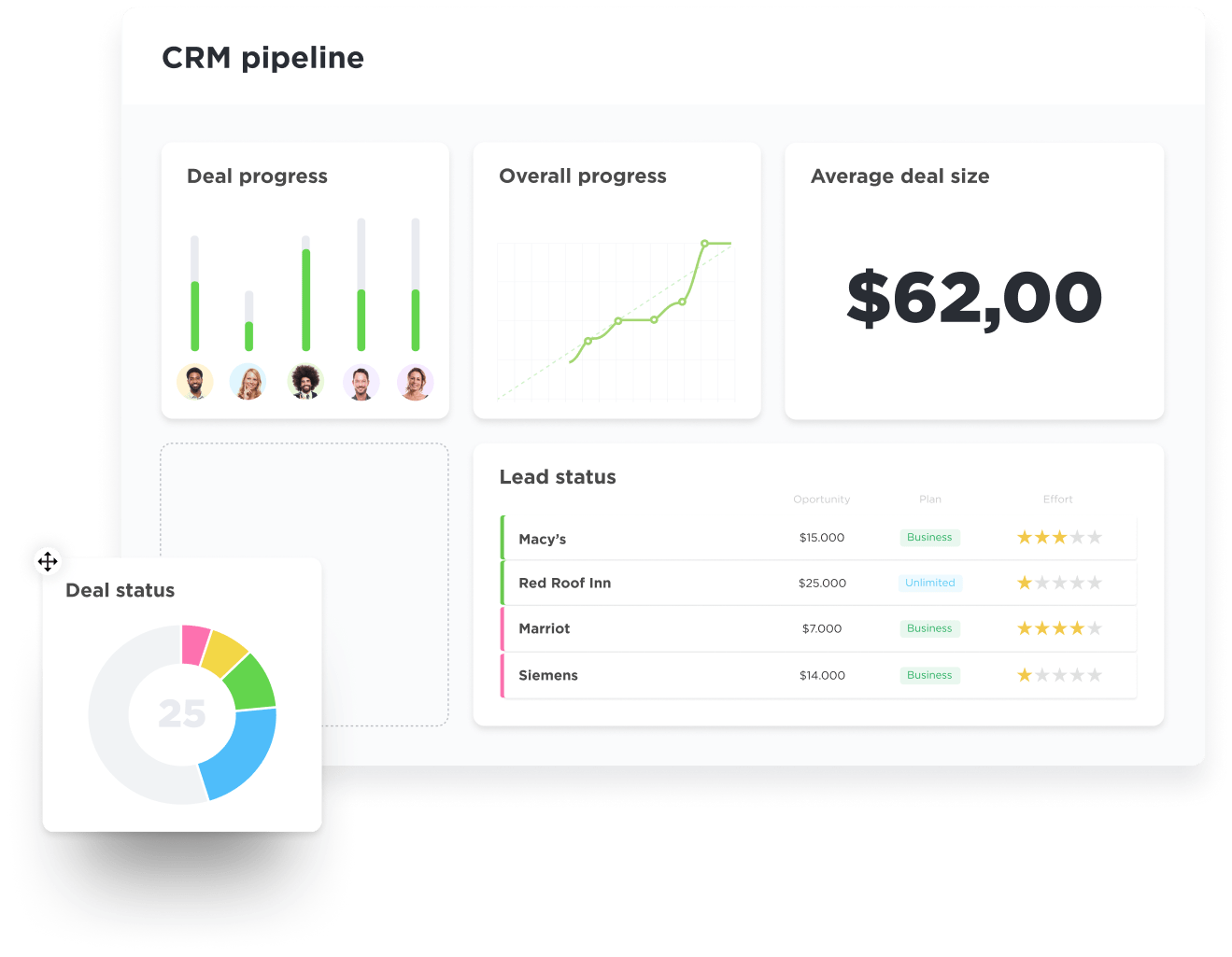
Challenges Medical Claims Processors Face Without a CRM
Handling medical claims without a CRM is like navigating a maze blindfolded. Critical details get lost, and delays pile up.
Here’s what often goes wrong when claims processors rely on manual methods:
- Client and payer contacts scattered — losing track of key representatives and follow-up commitments.
- Claim status updates lag — missing deadlines and creating backlogs.
- Communication gaps — emails, calls, and notes spread across unlinked platforms.
- Inconsistent documentation — lost or misplaced authorization forms and medical records.
- Difficulty tracking denials and appeals — no clear audit trail.
- Inefficient onboarding — new team members struggle without centralized history.
- Limited visibility into workflow bottlenecks — making process improvement nearly impossible.
- Lack of automated reminders — increasing risk of missed payments or claim expirations.
Why Traditional Claim Management Falls Short Compared to ClickUp CRM
Traditional Methods
- Contacts and claim notes scattered across emails and spreadsheets
- No centralized tracking of claim statuses or deadlines
- Manual follow-up reminders prone to error
- Difficulty managing denials and appeals
- Lack of integration with communication logs
- No clear visibility into team workloads
- Document storage is fragmented
- Limited automation leading to inefficiencies
ClickUp CRM
- Consolidate all provider, payer, and client information in one CRM
- Visual pipelines to track claims from submission to payment
- Automated reminders for deadlines and follow-ups
- Log calls, emails, and notes directly linked to claims
- Manage denials and appeals with transparent audit trails
- Dashboards to monitor team progress and bottlenecks
- Attach medical documents and authorizations to claims
- Leverage ClickUp Brain and Brain Max for intelligent insights and task automation
Unlock Powerful CRM Use Cases for Medical Claims Processors
Centralize Provider and Payer Contacts
Track Claims Through Every Stage
Manage Denials and Appeals Efficiently
Automate Follow-Ups and Reminders
Maintain Compliance with Document Management
Leverage ClickUp Brain Capabilities
Keeping Track of Journal Editors & Peer Reviewers
ClickUp organizes editors, reviewers, revisions, and deadlines, showing the full submission timeline at a glance.
Streamlining Industry Partnerships
Turning Meetings Into Follow-Up Actions
ClickUp attaches meeting notes to contacts, logs discussions, and turns next steps into tasks with owners and deadlines.
Who Benefits Most from ClickUp CRM in Medical Claims Processing
If You’re a Claims Processor Handling Multiple Payers
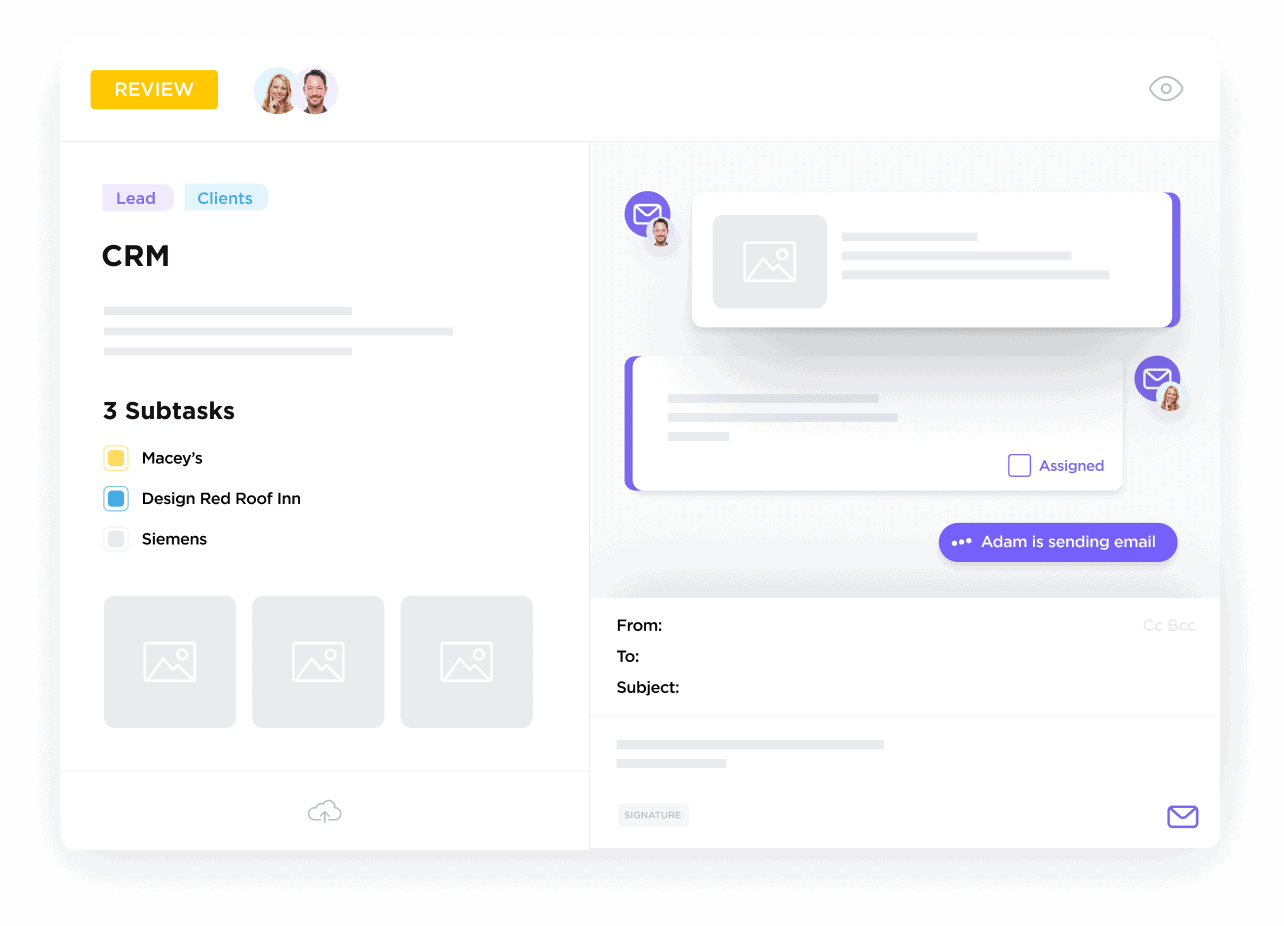
If You’re a Billing Specialist Managing Authorizations
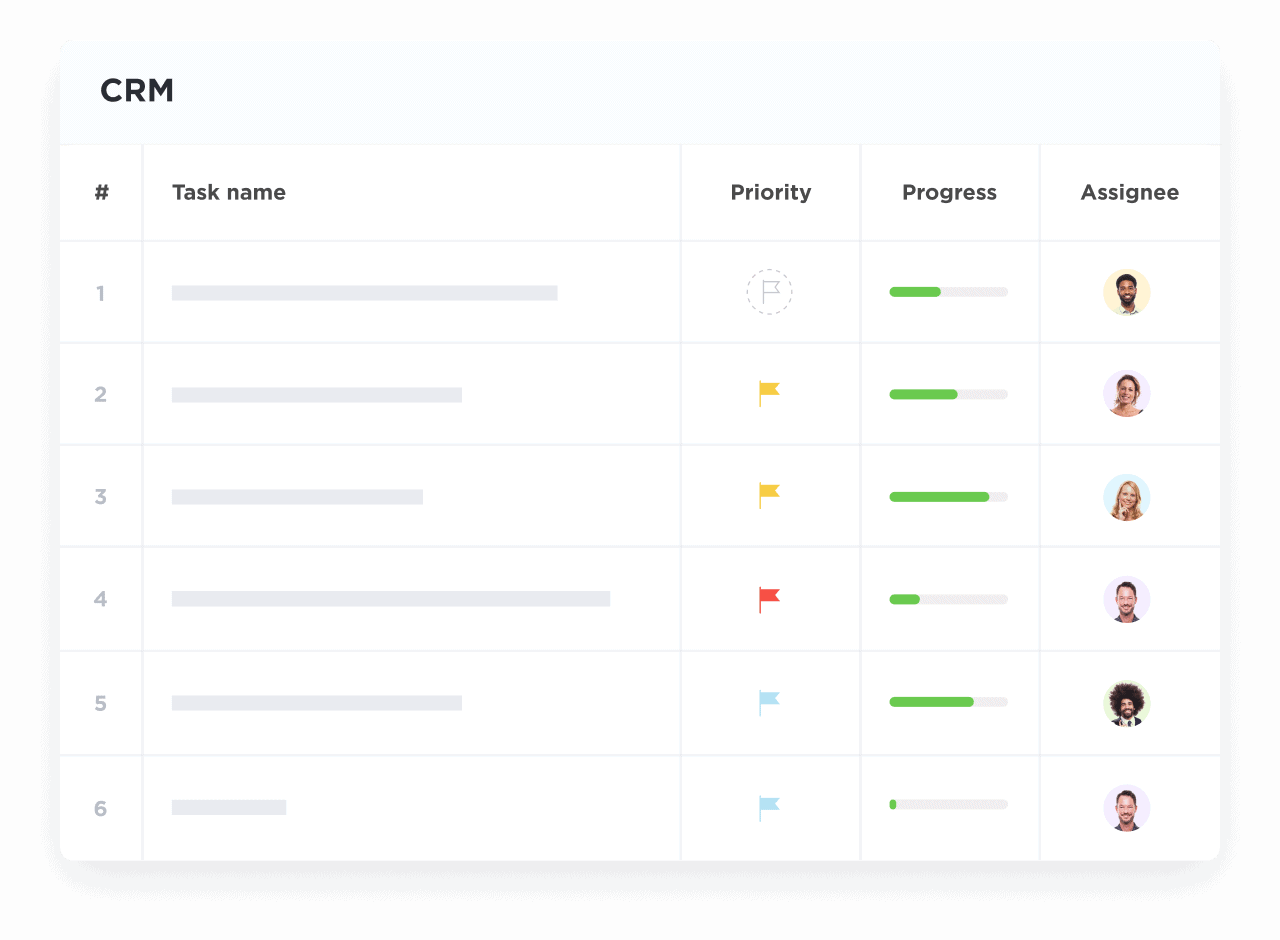
If You’re a Healthcare Administrator Overseeing Compliance

Six Steps to Master Medical Claims Processing with ClickUp CRM
1. Centralize All Contacts and Claim Data
Input providers, payers, clients, and claim details into a unified CRM database with custom fields and activity logs.
2. Build Visual Pipelines for Claim Tracking
Create stages representing claim submission, review, approval, denial, and payment to monitor progress at a glance.
3. Automate Alerts and Follow-Ups
Set automated reminders for deadlines, appeals, and client communications to keep your team proactive.
4. Attach and Manage Critical Documents
Securely upload authorizations, medical records, and correspondence directly to claims for easy reference.
5. Utilize ClickUp Brain for Insights
Leverage AI-powered recommendations to prioritize high-risk claims and identify workflow bottlenecks.
6. Monitor Performance with Dashboards
Track team workloads, claim aging, and resolution rates through customizable dashboards for continuous improvement.